Managing Meibomian Gland Dysfunction: A Complete Guide to MGD Care
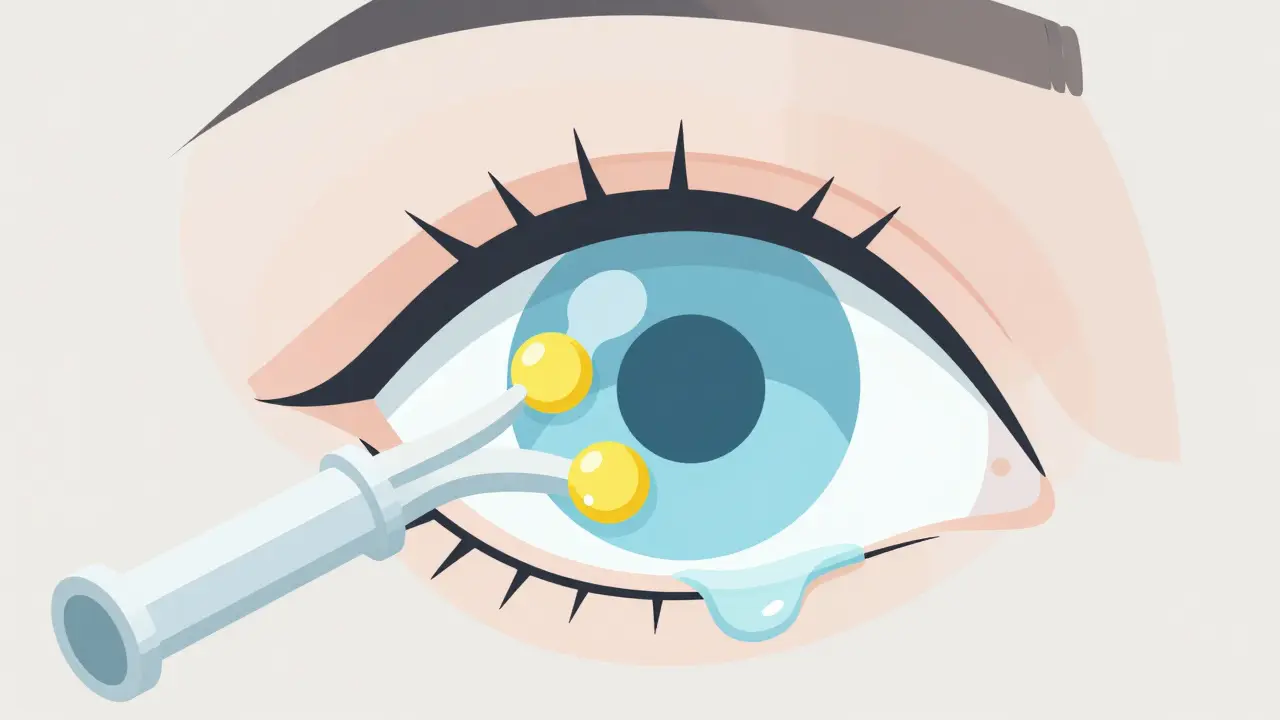
Understanding the Root of the Problem
To fix the problem, we have to understand what's actually happening inside your eyelids. Your eyes have a delicate balance of water and oil. The meibomian glands are responsible for producing the lipid (oil) layer. Without this oil, your tears evaporate almost instantly, leaving your cornea exposed and irritated. When we talk about MGD, we usually see two different versions. First, there is obstructive MGD, where the glands are physically plugged up-think of it like a clogged pipe. Then there is hypersecretory MGD, where the glands produce plenty of fluid, but the quality is poor, often too thick to flow properly. As we age, the prevalence of these issues spikes, which is why many of us start noticing a "gritty" feeling in our 40s or 50s. If left alone, these glands can actually atrophy, meaning they shrink and die, which can lead to permanent vision impairment or corneal damage.The Multimodal Treatment Approach
One thing you'll quickly learn from specialists is that there is no "magic pill" for MGD. The most successful results come from a multimodal approach-basically, attacking the problem from three different angles: mechanical clearing, inflammation reduction, and daily home maintenance.| Treatment | Primary Goal | Best For | Typical Cost (US) |
|---|---|---|---|
| LipiFlow | Thermal Pulsation | Obstructive MGD | $1,500 - $2,500 |
| IPL Therapy | Reduce Inflammation | Chronic Redness/Telangiectasia | $800 - $1,200 |
| MGP (Probing) | Physical Clearing | Severe Blockages | $750 - $1,200 |
| Daily Regimen | Maintenance | All Stages | Low (Product cost) |
In-Office Procedures: Clearing the Blockage
When home care isn't enough, doctors turn to medical devices to "reset" the glands. LipiFlow is one of the most well-known. It uses a device that applies controlled heat (about 42.5°C) to the inner eyelid while gently massaging the glands. This liquefies the hardened oils and pushes them out. Clinical data shows that this can significantly improve the expressibility of the glands, though the effects aren't permanent without follow-up care. Another powerful tool is Intense Pulsed Light, or IPL. Unlike thermal devices, IPL uses light wavelengths (500-1200 nm) to target abnormal blood vessels on the eyelid surface. By reducing these vessels, IPL lowers the inflammation that often keeps the glands blocked. Most experts suggest that IPL works best when combined with manual gland expression; using it alone often yields weaker results. For those with very stubborn blockages, Meibomian Gland Probing (MGP) might be suggested. This involves a specialist using a tiny probe to physically clear the duct. Many patients find that combining probing with a heat treatment like LipiFlow provides the most immediate and lasting relief because it addresses both the physical plug and the oil viscosity.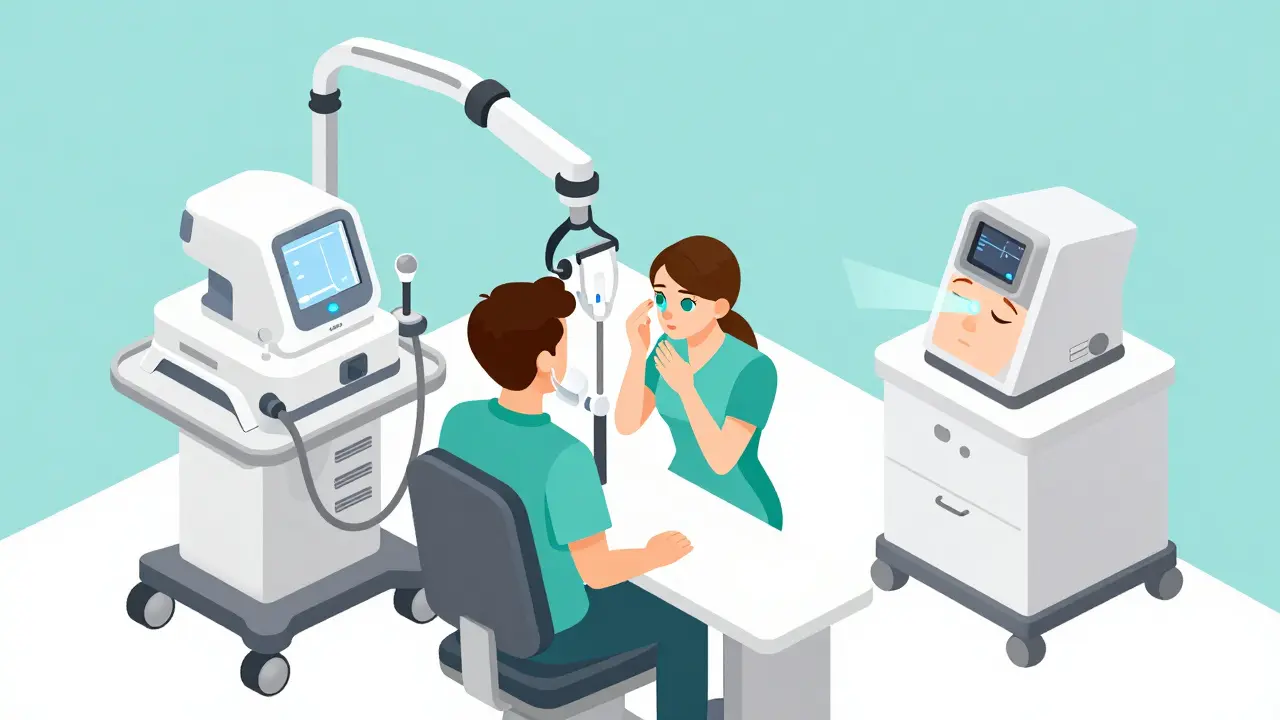
Pharmacological Interventions
Sometimes, the blockage is caused by a bacterial component or severe inflammation that mechanical clearing can't fix. This is where medication comes in. Interestingly, some antibiotics are used not just to kill bacteria, but for their anti-inflammatory properties. Research indicates that a short course of oral azithromycin (typically 5 days) can be more effective and better tolerated than a month-long course of doxycycline. It helps reduce the redness of the conjunctiva and improves the flow of the oil. On the topical side, medications like lifitegrast 5% have been shown to significantly reduce inflammation markers in advanced (Stage 4) MGD, which helps prevent further gland loss.The Non-Negotiable Home Care Routine
Here is the hard truth: you can spend thousands of dollars on in-office treatments, but if you don't do the home work, your symptoms will likely return within weeks. Specialists estimate that without daily maintenance, recurrence rates can exceed 60% within six months. Your daily 15-minute "eye gym" should look like this:- Warm Compresses: Use a dedicated mask (like a Bruder mask) heated to 40-42°C for about 5-10 minutes. This softens the oils in the glands.
- Lid Massage: Gently massage the eyelids to help the liquefied oil flow toward the surface.
- Lid Hygiene: Clean the lash line using a hypochlorous acid solution or an OCuSOFT scrub to remove debris and bacteria that can cause new blockages.

Managing Expectations and Costs
It's important to be realistic about what these treatments can do. If you have advanced gland atrophy-meaning you've lost more than 50% of your glands-the response rate to thermal therapies drops significantly. You can't "regrow" a gland that is completely gone, but you can maximize the function of the ones you have left. One of the biggest hurdles is the cost. Many insurance plans still view thermal evacuation as "experimental," leaving patients to pay out-of-pocket for expensive procedures. If you're budgeting for this, remember that a combination of one in-office procedure and a strict home routine is usually more cost-effective than repeated procedures without home care.Can MGD be cured permanently?
MGD is generally considered a chronic condition, meaning it cannot be "cured" in the sense that it disappears forever. However, it can be effectively managed. By combining in-office procedures like LipiFlow or IPL with a daily home regimen of warm compresses and lid hygiene, most people can achieve long-term symptom relief and prevent the progression of gland atrophy.
Which is better: LipiFlow or IPL?
It depends on your specific subtype of MGD. LipiFlow is generally superior for obstructive MGD (physically blocked glands) because it uses heat and pressure to clear the ducts. IPL is better for those with significant inflammation and abnormal blood vessels (telangiectasia) on the eyelid surface. Many patients benefit from a combination of both, as one clears the blockage while the other treats the underlying inflammation.
Are over-the-counter artificial tears enough?
Artificial tears provide temporary relief by adding moisture to the eye, but they don't treat the cause of MGD. Since MGD is an oil-deficiency problem, using only water-based drops is like trying to stop a leak by mopping the floor instead of fixing the pipe. You need treatments that target the meibomian glands to stop the evaporation process.
How often should I get professional MGD treatments?
There is no one-size-fits-all schedule. Some patients only need a single LipiFlow session every 6 to 12 months, while others may require a series of four IPL treatments every few years. Your doctor will determine the frequency based on your Ocular Surface Disease Index (OSDI) score and the level of gland atrophy seen on meibography.
Can I use a warm washcloth instead of a professional mask?
A washcloth often loses heat too quickly to effectively liquefy the oils inside the glands, which requires a consistent temperature of around 40-42°C for several minutes. Dedicated microwaveable masks (like the Bruder mask) hold heat much longer and provide a more consistent therapeutic temperature, leading to better results.




Comments (12)
Robin Walton
9 Apr 2026
Man, that gritty feeling is the absolute worst. It's so draining to deal with every single morning, but it's a relief to know there are actual paths to feeling better. Hang in there everyone!
Trey Kauffman
10 Apr 2026
Oh sure, just spend two grand to melt some eye grease. Truly the pinnacle of modern medicine. I'm sure the corporate overlords are thrilled we've found a way to monetize the basic act of blinking.
Danny Wilks
12 Apr 2026
It is quite fascinating how the biological complexity of the ocular surface often escapes the average person's notice until the dysfunction becomes debilitating, yet the sheer cost of these specialized thermal pulsation devices seems to create a significant barrier to entry for those who are not exceptionally well-insured in the current American healthcare landscape, which is a peculiar systemic irony when considering that the daily maintenance is actually the most critical component of long-term recovery.
Ben hogan
13 Apr 2026
Imagine thinking a microwave mask is some kind of revolutionary breakthrough. This whole guide is just a glorified sales pitch for overpriced gadgets that do exactly what a warm cloth did fifty years ago, provided you actually had the patience to use it.
Sarina Montano
14 Apr 2026
I've had a blast experimenting with the hypochlorous acid sprays! It's like a little spa day for your eyelids and it honestly cuts through the gunk way better than those old-school scrubs. If you're struggling with the 'sand' feeling, don't sleep on the Omega-3 supplements too-high-quality EPA/DHA can actually change the viscosity of your oil so it doesn't turn into glue in your glands. It's a total game changer when you combine the internal lipids with the external heat. Just a little tip from someone who's been in the dry-eye trenches for years!
Kelly DeVries
14 Apr 2026
omg i literally tried the bruder mask and it felt like my eyes were finally breathing again lol the struggle is so real when you just want to wake up without feeling like you slept in a desert
Julie Bella
15 Apr 2026
You guys are all just ignoring the fact that we are killin the planet with these disposible masks!! 🙄 why cant we just use real cloth and actually care about the earth while we fix our eyes lol its honestly so sad how people just buy whatever the doctor says without thinking about the waste 🌍😭
Simon Jenkins
16 Apr 2026
The sheer audacity of suggesting a washcloth is sufficient! We are talking about precise thermal thresholds here! If you aren't hitting 42.5 degrees, you are essentially just warming your skin while the glands remain frozen in a state of lipid stasis! It is an absolute tragedy that some people think they can DIY their way out of a clinical pathology!
Franklin Anthony
17 Apr 2026
funny how these doctors push the expensive machines when they know the 'maintenance' is the only thing that works. just another way to bleed us dry while they ignore the environmental toxins causing the inflammation in the first place lol
Victor Parker
18 Apr 2026
Exactly! The big pharma side of this is a joke 🤡 They don't want you to know that simple diet changes could stop this. Just keep paying for the IPL treatments forever! 🙄
Suchita Jain
18 Apr 2026
It is most distressing to see such a lack of discipline in the comments. One must adhere strictly to the prescribed medical regimen regardless of the cost, for the health of the eyes is a sacred trust. To neglect the daily cleaning of the lash line is a failure of personal responsibility that no amount of complaining can justify.
Lynn Bowen
20 Apr 2026
I've seen a lot of people in my community switch to the Bruder masks and they generally seem to prefer them over the cloths.