C. difficile Colitis: Antibiotic Risks and Fecal Transplant Explained
When you take an antibiotic for a sore throat or a sinus infection, you’re not just killing the bad bacteria-you’re also wiping out the good ones. And in some cases, that’s when things go seriously wrong. One of the most dangerous side effects isn’t nausea or a rash-it’s C. difficile colitis. This isn’t a rare glitch. It’s a growing public health crisis that sends half a million people to the hospital every year in the U.S. alone. For many, it starts with mild diarrhea. For others, it spirals into colon rupture, sepsis, or death. The real shock? The cure isn’t always more antibiotics. Sometimes, it’s poop.
How Antibiotics Trigger C. difficile
C. difficile, or C. diff, is a bacterium that lives quietly in some people’s guts without causing harm. But when antibiotics disrupt the balance of your gut microbiome, C. diff takes over. It multiplies fast, releases toxins, and attacks the lining of your colon. The result? Severe diarrhea, fever, abdominal pain, and in worst cases, toxic megacolon or a perforated colon.The problem isn’t just that antibiotics kill bacteria. It’s which ones you take. Not all antibiotics carry the same risk. A major 2023 study tracking over 33,000 hospital stays found that certain drugs are far more dangerous than others. Piperacillin-tazobactam-a common broad-spectrum antibiotic-carried more than double the risk of C. diff compared to other drugs. Carbapenems and later-generation cephalosporins like ceftriaxone were just as risky. Even more telling: each extra day on antibiotics raised your risk by 8%. After 14 days, the danger shot up again. That’s not a coincidence. It’s a pattern.
On the other end of the spectrum, tetracyclines like doxycycline showed the lowest risk. Clindamycin, once a go-to for dental infections, is now known as one of the worst offenders. The CDC calls this “antibiotic-associated diarrhea” for a reason-it’s not random. It’s predictable. And it’s preventable.
The Hidden Danger: Asymptomatic Carriers
Here’s something most people don’t realize: you don’t have to be sick to spread C. diff. About 5% of healthy adults carry the bacteria without symptoms. In hospitals, that number jumps to 20%. These people are silent carriers. They don’t have diarrhea. They don’t feel ill. But they shed spores in their stool-and those spores can survive for months on surfaces like bed rails, toilets, and doorknobs.What’s terrifying is that for these carriers, antibiotics don’t increase their risk of getting sick. A 2024 study found their baseline risk was already 27 times higher than non-carriers. Antibiotics didn’t push them over the edge-they were already on the edge. That means traditional stewardship-cutting back on antibiotics-won’t stop C. diff in these cases. We need new tools. Probiotics? Not proven. Monoclonal antibodies? Still being tested. The real breakthrough? Restoring the gut.
Fecal Transplant: The Unlikely Cure
In 2013, a study published in the New England Journal of Medicine changed everything. Researchers compared two treatments for people with recurring C. diff: standard vancomycin (an antibiotic) and fecal microbiota transplantation (FMT). The results were shocking. Vancomycin worked in only 31% of cases. FMT worked in 94%. One infusion cured most. A second infusion cured almost everyone.How does it work? You take stool from a healthy, rigorously screened donor. You process it, filter out solids, and deliver it-via colonoscopy, enema, or oral capsule-into the patient’s colon. The idea isn’t gross (though it sounds that way). It’s biological. You’re not transplanting waste. You’re transplanting trillions of healthy bacteria. These good microbes crowd out C. diff, restore balance, and rebuild the gut’s natural defenses.
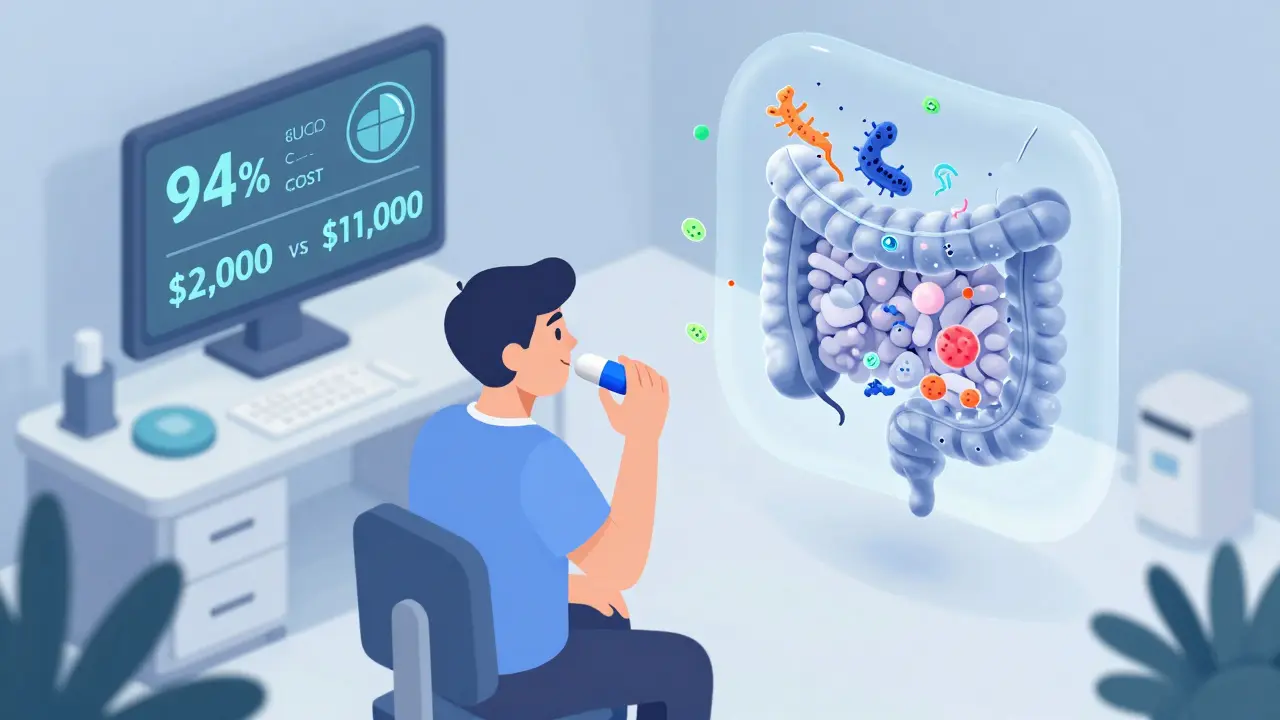
Today, FMT isn’t experimental. It’s recommended by the American Gastroenterological Association for anyone who’s had three or more C. diff recurrences. Success rates? 85% to 90%. That’s better than any drug. And it’s cheaper than repeated hospital stays. One hospitalization for C. diff averages $11,000. An FMT? Around $2,000.

From Poop to Pills: The New Generation
You don’t have to drink a shake of someone else’s stool anymore. In 2022 and 2023, the FDA approved two standardized FMT products: Rebyota and Vonjo. These are oral capsules packed with carefully selected, tested, and frozen donor material. No colonoscopy. No mess. Just swallow a pill. These aren’t magic bullets-they’re the first step toward precision microbiome therapy.Even more exciting? Drugs like SER-109, a capsule made from purified bacterial spores, showed 88% effectiveness in late-stage trials. It’s not fecal matter. It’s a targeted cocktail of the exact microbes that fight C. diff. No donor needed. No stool processing. Just science.
These aren’t just alternatives. They’re the future. And they’re already here.
What You Should Know If You’re on Antibiotics
If you’ve been prescribed an antibiotic, here’s what to ask your doctor:- Is this antibiotic really necessary? Sometimes, viral infections don’t need antibiotics at all.
- Can we use a narrower-spectrum drug? Tetracyclines or penicillin might be safer than piperacillin-tazobactam.
- How long do I really need to take it? Most courses can be shortened without losing effectiveness.
- Am I at risk for C. diff? If you’ve had it before, or if you’re over 65, your risk is higher.
And if you’ve had multiple C. diff infections? Don’t accept more antibiotics as the only answer. Ask about FMT. It’s not experimental. It’s not fringe. It’s the most effective treatment we have for recurring cases.
Why This Matters Beyond the Hospital
C. diff isn’t just a hospital problem anymore. Since 2011, community cases have risen by 14% every year. People who’ve never been hospitalized are getting sick. Why? Because antibiotics are everywhere-in livestock, in water, in overprescribed prescriptions. One study found nearly half of community C. diff patients had taken antibiotics within the last 30 days.What’s happening in the U.S. is happening here too. In the UK, NHS data shows rising C. diff rates outside hospitals. Antibiotic stewardship programs are working in some places, but not everywhere. And the more we rely on broad-spectrum drugs, the more we risk creating a cycle of infection, recurrence, and treatment failure.
The answer isn’t to stop using antibiotics. It’s to use them smarter. Shorter. Narrower. And when they fail, we need better options. FMT isn’t a last resort. It’s a smart first choice-for the right patients.
Can C. difficile go away on its own?
Yes, in mild cases, especially if you stop the antibiotic that caused it. Your body’s natural immunity can sometimes clear the infection without treatment. But this only works if symptoms are mild and you’re otherwise healthy. If you have fever, severe pain, or bloody diarrhea, don’t wait. Seek medical help immediately.
Are probiotics effective for preventing or treating C. diff?
The evidence isn’t strong enough to recommend probiotics for C. diff prevention or treatment. Some studies show slight benefit, but others found no effect. Worse, in immunocompromised people, probiotics have been linked to dangerous infections like bloodstream infections. The IDSA and CDC both say probiotics shouldn’t be used routinely. Stick to proven treatments.
How is a fecal transplant done today?
Most often, it’s done as an oral capsule you swallow. These capsules are FDA-approved, contain screened donor material, and don’t require a colonoscopy. In some cases, it’s delivered via enema or colonoscopy, especially if the patient has other bowel issues. The procedure is quick, usually takes less than an hour, and most people go home the same day.
Who qualifies for a fecal transplant?
FMT is recommended for adults who’ve had at least three episodes of recurrent C. difficile infection that didn’t respond to standard antibiotic treatment. It’s also considered for severe or fulminant cases that don’t improve with antibiotics alone. It’s not used for first-time infections unless they’re life-threatening.
Is fecal transplant safe?
When done with screened donor material-like the FDA-approved capsules-it’s very safe. Donors are tested for over 50 infectious diseases, including HIV, hepatitis, and drug-resistant bacteria. The risk of serious side effects is less than 1%. Long-term risks, like changes in metabolism or immune function, are still being studied, but no major issues have been found in over a decade of use.
Can C. difficile come back after a fecal transplant?
Yes, but it’s rare. About 10-15% of people experience another recurrence after FMT. This usually happens if the original cause-like ongoing antibiotic use or a weakened immune system-isn’t addressed. FMT restores the gut, but it doesn’t make you immune. Avoid unnecessary antibiotics, and follow up with your doctor if symptoms return.




Comments (9)
Michael FItzpatrick
26 Feb 2026
Let me tell you something wild-our guts are basically sci-fi ecosystems, and we’ve been treating them like a junkyard. Antibiotics? More like a flamethrower in a library. I’ve seen patients go from ‘mild tummy ache’ to ICU in 72 hours because someone thought ‘broad-spectrum’ meant ‘better.’ But here’s the kicker: the real heroes aren’t drugs. They’re microbes. Trillions of them. Tiny, ancient, silent warriors that evolved alongside us. FMT isn’t gross-it’s poetic. We’re not dumping poop. We’re rebooting a civilization. And yeah, I’ll say it: if you’ve had three recurrences and your doc still says ‘take more vancomycin,’ find a new doctor. This isn’t 1998 anymore. We’re in the microbiome renaissance.
Brandice Valentino
27 Feb 2026
ok so like… i just read this whole thing and im like… wow. i mean. poop. as medicine. 🤯 i know its like… scientifically valid and all but… its still… poop. like. imagine your grandma’s toilet bowl… being filtered and turned into… pills. and now im just… imagining the smell. like… what if the donor had eaten tacos the night before? is that… in the quality control? lol. also. why do they even need to do colonoscopies anymore? why not just… inject it through the nose? like… why not just… make it a smoothie? i’m not even being serious. but also. i am.
Larry Zerpa
27 Feb 2026
Let’s cut through the hype. FMT works? Fine. 94%? That number is statistically dubious. The 2013 NEJM study had a sample size of 16 in the FMT arm. That’s not a breakthrough-it’s a pilot. And let’s not ignore that 10-15% recurrence rate after FMT is just as high as some antibiotic regimens. Also, where’s the long-term data? Five years? Ten? We’re transplanting entire microbial ecosystems into people who may later develop IBD, diabetes, or obesity. Are we sure we’re not creating tomorrow’s epidemics? And don’t get me started on the FDA-approved capsules. They’re just corporate rebranding of a procedure that’s been around since ancient China. This isn’t innovation. It’s repackaging. And the media? They’re selling snake oil with a lab coat.
Ashley Johnson
27 Feb 2026
They’re lying. All of it. The CDC, the FDA, the hospitals-they’re all in on it. FMT? It’s a cover. The real cure is in the government’s secret bio-labs. They’ve been injecting people with synthetic gut flora since 2010. Why? To control our digestion. To make us docile. You think antibiotics are bad? Wait till you find out what’s really in your probiotic gummies. I’ve been tracking the rise in C. diff since 2011. Coincidence? No. It’s a rollout. They want us dependent on pills. And now they’re selling ‘capsules’ like it’s medicine. It’s not. It’s a Trojan horse. They’re not fixing your gut. They’re mapping it. And your microbiome? It’s your soul. They’re stealing it.
tia novialiswati
1 Mar 2026
Yessss this is so important!! 🙌 I had a cousin go through 4 rounds of C. diff and was in tears every time she had to go to the hospital. When she finally got FMT? She cried happy tears. Like… she went from bedridden to hiking in the mountains in 3 weeks. 🥹 I know it sounds weird but it’s literally life-changing. If you’re struggling with this, PLEASE ask your doctor about it. You don’t have to suffer. There’s hope. And it’s not magic. It’s science. And it works. 💖
Lillian Knezek
2 Mar 2026
They’re putting GMO poop in capsules. 😳 I read somewhere the donors are paid to eat only organic kale and kale smoothies for 6 months before donation. Why? So they can control the bacteria. Who’s paying them? Big Pharma. The same people who make the antibiotics. It’s all connected. They make the problem… then sell the cure. And they call it ‘science.’ I’m not taking those capsules. I’d rather drink my own… filtered… juice. 🤢
Maranda Najar
4 Mar 2026
Oh, the poetry of it all. The tragedy. The sublime absurdity of modern medicine. We have become so detached from the natural order that we must now, with clinical detachment, administer the very waste of another human being-filtered, frozen, sterilized-into the sacred chambers of our own intestines… just to survive. And we call it progress. We call it innovation. We call it science. But I ask you: what have we become? A species that no longer trusts its own body… so we import salvation from the bowels of strangers? This is not healing. This is desperation dressed in white coats. And yet… I weep. Because for the first time, someone is listening. Someone is offering not just a cure… but dignity. And isn’t that worth more than a thousand antibiotics?
Christopher Brown
5 Mar 2026
USA leads. Rest of the world still uses antibiotics. That’s why we have lower mortality. FMT? Fine. But don’t compare us to Europe. We don’t have your healthcare bureaucracy. We fix problems. You debate them.
Sanjaykumar Rabari
5 Mar 2026
C. diff is fake. It's made by big pharma to sell more drugs. I read it on a forum. No one dies from poop. Only from vaccines.